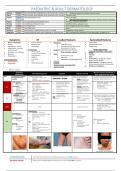
PAEDIATRIC & ADULT DERMATOLOGY
Macule <1cm Non elevated/ Non-Palpable lesion of altered colour change • Erythema toxicorum, roseola, pityriasis rosea
Patch >1cm Non elevated/ Non-Palpable lesion of altered colour change Psoriasis, tinea
Papule <1cm Elevated/Palpable lesion Warts, SCC/BCC,
• RED FLAG (Maculopapular)= Meningitis, Rubella, Measles, KawasakI
Plaque >1cm Flat topped/Elevated/Palpable lesion Psoriasis, seborrheic dermatitis
Nodule >1cm Solid/Elevated/Palpable lesion SCC/BCC, lipoma, sebaceous cyst
Vesicle <1cm Fluid filled lesion HSV, shingles/chicken pox, cellulitis
Bulla >1cm Fluid filled lesion Burns
Urticaria >1cm Raised white or reddened itchy rash across body Anaphylaxis, drug-reaction
Petechiae <1cm Pinpoint darkened spots due to bleeding on superficial skin HSP, meningococcal septicaemia (non-blanching), Leukaemia, ITP
Symptoms RF Localised features Generalised features
• Where / distribution • Chronic Illnesses 1. Asymmetry • Lymph Nodes
• Pruritis • Sexual History a. Flexural/Extensor • Neurovascular status
• Pain (which is worse?) • FHx of atopy b. Sun exposed/Clothing Covered • Temperature
• Inflammation = red, hot, c. Dermatomal vs Truncal
Environmental 2. Border: Round/Oval/Annular/Reticular Koebner phenomenon
swollen, painful
• Recent Travel a. Ulcer ® erosion ® fissure “lesions at site of injury – skin scrape”
• Discharge – pus, bleeding
• Insect & Plant Exposure 3. Colour 1. Vitiligo
• Blistering
• Drug Exposure a. Erythematous, Scaly 2. Psoriasis
• B Symptoms 3. Warts
• Hobbies b. blanching
• Ill contacts c. Hypopigmented/Hyperpigmented 4. Lichen planus – polygonal or planus
Exacerbating factors purple, pruritic, plaques
Ø Autoimmune hx • Pets 4. Diameter
• Chemical Exposure 5. Evolution 5. Lichen sclerosis – hourglass shape dry
Ø Propranolol thinned autoimmune skin inflammation
6. Raised / vesicular vs pustular or flat
7. Smooth vs rough 6. Mollascum contagiosum
RED FLAGS
Erythema Steven Johnson Syndrome vs
Non-blanching rash Cellulitis Urticaria (hives)
Multiforme toxic epidermal necrolysis
Def Itchy Red rash caused Bleeding under the skin Bacterial Infection of BOTH Rash caused by histamine SJS and TEN = spectrum of same
by Hypersensitivity Ø petechiae (< 3mm) = burst lower dermis + SC tissue. release from mast cells: pathology (disproportionate immune
reaction capillary Ø Acute - anaphylaxis response) = epidermal necrosis
Ø Purpura (3-10mm) = leaking BV (allergy), insect bites,
Viral infections DDx: Ø Immunocompromised meds, skin rubbing • Meds (ABx, allopurinol, anti-
Ø HSV (cold sore) Ø Meningococcal septicaemia Ø Recent travel -high risk (dermatographism), viral epileptics, NSAIDs)
Ø Mycoplasma Ø HSP – PAPAH areas (underwater infections • Infections (HSV, CMV, HIV,
Medications Ø ITP – post-viral swimming, travelling Ø Chronic - idiopathic, mycoplasma)
RF Ø Penicillins Ø Acute leukaemia bushes) sunlight, exercise, hot or • HLA genetic types
Ø NSAIDs Ø HUS – oliguria, aneima, Ø Chronic illness cold weather, strong
Ø Anti-convulsants diarrhoea emotions, autoimmune
Ø Recent trauma
(phenytoin) Ø Mechanical – SVC distribution (e.g. SLE)
Target lesion (strong cough, vomit) – mostly Ø Painful unilateral red
DOES NOT affect MM around neck and eyes inlafmfed limb Blistering and shedding of top layer of
Ø NAI • Red small itchy patchy
but does cause sore DDx: erysipelas = only skin on lips and MM (e.g. eyes, lungs)
Ø Viral illness – influenza, lumps
Sx mouth (stomatitis) epidermis ® Leads to skin shedding days after
enterovirus • Assoc. w/ angioedema
Arthralgia SJS = <10% of body SA
and skin flusing
Headache TEN = > 10% of body SA
Flu-like symptoms
• 2nd infection = skin breaks causes
cellulitis and sepsis
COMP. Death Cellulitis and sepsis • Permanent skin damage +
scarring
• Vision loss – if eye involvement
Identify cause:
Ø Check BP – HSP, HUS
Supportive mx
Ø FBC, EUC, LFT, CRP, ESR, Coag Acute urticaria
Ø If clear cause
(Leukaemia, infection)
• IM adrenaline (if
Ø Blood culture
If unclear cause anaphylaxis)
Ø UA
Ø CXR – Medical emergency
Ø LP
mycoplasma Chronic urticaria: Ø Steroids
Rx Mx: •
• Antihistamines Ø IVIg
Ø Rx underlying cause
If severe • PO steroids Ø immunosuppressants
Ø ABCDE – IV 1g ceftriaxone (HiB,
Ø Admit • Anti-leukotrienes (e.g.
gram -ve)
Ø IVF, analgesia montelukast)
Benzyl – Neisseria, pneumo,
Ø +/- ABx or
GBS, listeria
antivirals
Ø Notify health department if HIB
and meningitis
*TARGET LESIONS
(ERYTHEMA MULTIFORME)
LIVEDO RETIUCLARIS MOTTLED NET-LIKE DUE TO SWOLLEN BV assoc. to COLD exposure
ERYTHEMA AB IGNE RETICULAR HYPERPIGMENTATION DUE TO LONG-TERM HEAT exposure
, PSORIASIS + DDx
Pathogenesis [not curable] Risk factors Clinical features General Rx
• Chronic autoimmune skin condition (2-3%) • Streptococcal infection • +/- onycholysis, koilonychia, ridging Conservative
• hyperproliferation of keratinocytes and precipitate guttate psoriasis (50%) • Reduce sun exposure
inflammation due T-cell immune (Esp. in children) • Dry flaky scaly well-demarcated red • Avoid smoking, alcohol
dysregulation (release of inflammatory • Trauma – localises psoriasis plaque with silvery scale ® affects • Reduce stress
cytokines ® IL1B, TNFa and IL17A) (Koebner phenomenon) extensor surfaces (e.g. elbows and Medical
• Bimodal distribution (15-25yo and 50-60 • Excess alcohol consumption knees) + scalp, lower back
• Topical steroids
yo) • Medication (BB, • Mild itching
• Topical vit D analogues
• 1 in 3 psoriasis patients suffer from hydroxychloroquine, NSAIDs, • Auspitz sign = small bleeding points (calcipotriol)
psoriatic arthritis prednisone withdrawal) after psoraitc plaque removed
• Topical tacrolimus (calcineurin)
• Strong familial & genetic disposition • MetSyn • DDx: eczema (itchy, has skin thinning) – only in adults
(30%) – 1st deg relatives • Stress (emotional + physical) • Phototherapy or narrow band
*Psoriasis Area and Severity Index (PASI) = UVB – for extensive guttate
assess psoriasis based on redness, thickening psoarisis
and scaling
Scalp psoriasis Guttate Pustular Psoriasis Chronic plaque psoriasis Inverse (flexural) Erythordermic psoriasis
(classical) (droplet-like psoriasis) psoriasis
• Diffuse or well- • Acute onset of widespread • Rare = pustules under • Most common (90% in • Found under folds • Rare dermatological
circumscribed small plaques (often on red skin psoriasis patients) (armpits, groins, emergency (Acute +
plaques trunk) • Confined to palms and • Thick well-defined red breasts) chronic)
• 2-3 wks after streptococcal soles ® scaling red scaly plaques ® • Sharp-edged patches • Red inflamed psoriasis
throat infection ® mostly • Triggered by extensors + lower back (no scaling) areas whole body
young adults withdrawal of systemic • Auzpitz sign (bleeding) • Systemic illness causing
steroids when plaque removed temp. dysregulation,
electrolyte disturbance,
cardiac failure
Steroid lotions 1) Phototherapy Treatment resistant Treatment resistant Oral meds to control
2) Topical CS symptoms
3) ENT referral +
tonsillectomy
Differential Dx:
Tinea (Ringworm) Pityriasis rosea Intertrigo Seborrheic dermatitis
“cradle’s cap”
Def Fungal infection of the skin (dermatophytosis) • Generalised Self limiting rash • Irritant dermatitis Inflammatory condition affecting
Ø Well-demarcated itchy red scaly annular (with 3/12) (confused with sebaceous glands ® usu. found in
patch or plaque • NOT contagious flexural psoraisis) scalp, eyebrows and nasolabial folds
DDx: pityriasis versicolor
• XS sweat • Post-viral URTI • Not showering • 10% if infants (3 wks - 12 mths)
• Occlusive clothing • Not removing
RF • Chronic illness clothing
• Poor hygiene
• Tinea capitis = scalp + hair loss • Herald small scaly oval red • Inflammed red skin • Greasy rash
• Tinea pedis “athlete’s foot” = foot (between rash/patch on trunk – with fissuring and • self-limiting and usu. resolved
toes) • Xmas tree distribution Along peeling by 4 mths old
• Tinea cruris = groin langer’s lines (skin creases) • Moist areas of body •
Sx • Tinea corporis = body • Low grade Fever
• Onychomycosis = fungal nail infection • Malaise, Fatigue
(thickened, discoloured and deformed nails) • Headache
• Arthralgia, sore throat
• Scrap scales ® M/C/S • Self-limiting Psudo cream Conservative
Conservative • Continue normal ADLs (not • Gentle emollient = mineral oil
Ø Loose breathable natural clothing contagious) Medical
Ø Keep area clean, dry • If itchy ® emollients, topical, • Scalp = Ketoconazole shampoo
Ø Use separate towel, new socks sedating antihistamines (left on for 5 minutes before
Ø Avoid scratching and spreading to other areas (chlorphenamine) washing off)
Medical • Face & body - Anti-fungal
• Topical antifungals (minimise steroid combos) topical up to 4 weeks +/- topical
® risk of cataract hydrocortisone 1% for inflamed
o LAMISIL = Athlete’s foot areas and itch
o Pevaryl – back If unresponsive
• Hydrozole (only if itchy BUT avoid 1st ) ® • Refer to dermatologist
steroid may mask an underlying fungal
infection ® tinea incognito
Rx • Amorolfine nail lacquer for nail infections for
6-12 months
• PO terbinafine (if resistant -monitor LFTs)